What is Remote Patient Monitoring (RPM)?
In its simplest definition, RPM or Remote Patient Monitoring is the use of technology that allows for healthcare to be provided to patients at a distance. In other words, RPM simply entails using technology to collect, transmit, and analyze patient health data. Whether from home, or another remote setting external to a traditional clinic, RPM makes it possible to manage health without the added barriers created by physical care.
In addition to providing convenience, RPM improves accessibility to healthcare, and has been shown to increase care quality and lower health risk.
Remote Patient Monitoring also makes it possible to better tailor care to the lived realities of patients and the diseases they manage. Many studies support this benefit, with RPM programs used for conditions both chronic and temporary seeing measurable improvements in patient health outcomes.

What’s the Difference Between RPM and Telehealth / Telemedicine?
Now that we’ve established what RPM is, let’s define what it isn’t. Remote Patient Monitoring is commonly confused, or used interchangeably with, the term Telemedicine. This is in fact highly inaccurate and misleading, as these terms have entirely different definitions and regulatory frameworks.
Telehealth is a broad term that refers to the entire industry of health service provision via telecommunication technologies. Remote Patient Monitoring (RPM) and Telemedicine are two separate models of care, which both fall under the umbrella of Telehealth.
Telemedicine refers specifically to clinical services that are provided through remote technology. This could look like a doctor in a small-town or remote community consulting with a needed specialist from a distance. Other forms of telemedicine could include transmitting health records to external medical centers and specialists to allow patients to access health resources they could not have otherwise acquired.
Remote Patient Monitoring, in contrast, can include non-clinical health services in addition to clinical services. This form of care is a highly specific subset of Telehealth, and differs in application to telemedicine.
When Did Remote Patient Monitoring (RPM) Begin?
RPM already has several wide-spread applications in medicine. Many diseases, specifically chronic conditions, already rely on remote forms of monitoring and data collection to effectively manage care. In fact, technically speaking, RPM is not exactly new. Even care provided entirely over the telephone can be classified as Remote Patient Monitoring. In this sense, the US has already integrated telehealth in many ways throughout its healthcare system.
Telemedicine technology was first introduced in the1960s due to the needs of the National Aeronautics and Space Administration (NASA) and the Nebraska Psychology Institute, according to researchers from Saint Louis University and Bentley University and published in theInternational Journal of Environmental Research and Public Health.
In the 1970s, the Kaiser Foundation International teamed up with Lockheed to create a remote monitoring system capable of providing healthcare delivery to a rural location that lacked basic medical services.
Medical staff were then able to send patient information from the remote monitoring tools to a hospital or medical facility many miles away from the original site. The expected outcome would allow rural areas around the world to receive better healthcare services and improve patient health.
What are some examples of Remote Patient Monitoring (RPM)?
While RPM has existed in some basic form for a while, as telehealth technology has advanced, so have the tools used to remotely monitor patients in safer, more effective ways. Today, the devices and systems used in effective Remote Patient Monitoring provide 24/7 observation, alerting, and clinical support.
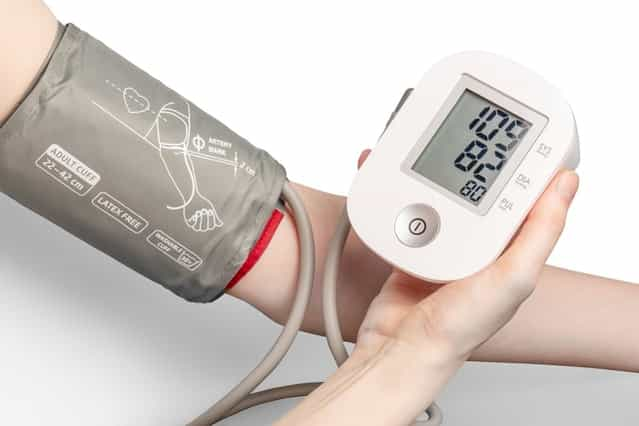
Common contemporary examples of Remote Patient Monitoring (RPM) include cellular-enabled biometric monitoring devices that continuously and accurately collect and analyze health data. This includes everything from blood pressure and glucose levels to weight fluctuations and signs of allergic reaction, in addition to many other critical health insights.
What Are Some Common Applications of Remote Patient Monitoring?
While RPM has many contemporary applications, the benefits of Remote Patient Monitoring have made enormous strides in the management of chronic conditions. Chronic diseases, such as diabetes, hypertension, heart disease, and many more, affect nearly half of the American population.
Chronic conditions also account for the highest expenditures and burdens on our healthcare system. These facts illustrate the critical need for effective, accessible treatment models that accommodate the lived realities and limitations of over 133 million Americans.
Diabetes management is one example of enormously successful applied RPM. Patients suffering from this disease must be in constant awareness of their blood glucose levels, and must act quickly when levels become irregular. Without consistent observation of these frequently fluctuating levels, life-threatening complications are likely to occur.
Remote Patient Monitoring provides a unique solution to this incurable, high-risk disease. Professional RPM providers, such as Accuhealth, provide devices and platforms that create consistent data transmission, and that send alerts to both patients and their providers when readings become irregular or require medical intervention.
Diabetic patients using RPM services are best treated through the use of a 4G LTE connected glucometer that transmits data directly from patient to doctor. This reduces the risk and occurrence of emergencies, including fatal complications.
Hypertension, also known as high blood pressure, is another example of how RPM can not only provide adequate care, but it can actually improve care quality over traditional methods. One third of Americans will suffer from hypertension in their lifetime. This wide-spread health crisis is in desperate need of effective treatment solutions.
The lack of visible symptoms associated with high blood pressure makes it a challenging disease to manage. leading to common life-threatening issues amongst patients such as heart attacks and strokes.
Fortunately, the realities of treating high blood pressure fit perfectly with the benefits Remote Patient Monitoring provides. Traditionally, patients with hypertension were required to go to clinical settings to have their blood pressure assessed, and then manually record their levels at home. This results in missed readings, and recurring misinterpretation of data, which increases the risk of emergencies.
Today, RPM provides a much better solution: around the clock monitoring and data transmission of blood pressure readings, all without leaving the house. With this model, the tedious and often inaccurate process of patients manually noting and tracking biometric readings is removed, lowering risk and empowering both patients and providers in managing and improving health.
Remote Patient Monitoring (RPM) – Summary
Remote Patient Monitoring is defined as using technology to provide care to patients at a distance. Unlike the much more specific field of Telemedicine, RPM is not relegated to clinical services only. Patients requiring non-clinical care can also benefit from the many applications of Remote Patient Monitoring, and providers can use these tools to effectively improve quality care and life for their patients.
Find out more about Remote Patient Monitoring, and how RPM providers like Accuhealth are facilitating the easy, scalable implementation of RPM programs for patients and providers across the United States, at accuhealth.tech.