Introduction
Without solid, reliable devices, we cannot do any of this, which makes this part of the patient monitoring/telehealth conversation extremely important.
Your patients have to have a seamless experience. Your staff needs to make the use of the devices look as easy as possible. Ultimately, devices need to be the easiest part of the remote patient monitoring puzzle.
Without them, healthcare providers will have no chance of capitalizing on everything patient monitoring offers.
So, in this post, we will cover everything from the basics, like what these devices are and examples of them, to the nitty-gritty details, such as FDA standards, Bluetooth versus cellular devices, and how you make the best decision for your practice.
What Is a Remote Patient Monitoring Device?
Most of us are incredibly familiar with remote patient monitoring devices at this point. You might even be wearing one as you read this—especially if you’ve got on a Fitbit or an Apple Watch. These are devices that have sensors that will track specific physiological parameters and convert them into data you can understand and interpret. In general, they are Bluetooth and have to connect to a cellular device to work.
But the largest difference is that your watch doesn’t report that back to medical professionals. Particularly, they don’t track physiological parameters and wirelessly transmit them to a centralized apparatus. Ours is called Evelyn.
That apparatus is where doctors and other professionals involved in care can analyze the data and use it to fine-tune their efforts.
Another big difference between remote patient monitoring devices and the wearable devices you are familiar with is that patient monitoring devices are often dedicated to one specific purpose—which we will cover later. Essentially, if a sensor can track data that provides a granular look at a certain health condition or ailment, there is most likely an RPM device for that condition or ailment.
What Makes For Great RPM Devices?
There are a lot of devices out there, but not all remote monitoring devices are created equal. We encourage you to consider some factors before committing your practice to one remote patient monitoring device over another.
Namely, there are five factors, including
- Ease of use
- Bluetooth vs. Cellular
- Live Interaction
- Storage and Forwarding
- Integration
Ease of Use, for Patients and Providers
It’s hard to get people to prioritize their health, especially if the equipment is difficult to use. That’s why a great remote patient monitoring device needs to be as easy to maneuver as possible. Additionally, it would be helpful if the device was coupled with comprehensive patient portals that are accessible 24/7. Then the patients can view their medical data and let them communicate with their medical providers.
While you and your colleagues may need to interpret that data further, the RPM device delivers granular data on the patient. Whenever patients have direct access to this information, they are more likely to make better health choices because they see the results in real-time in a format that is easy for them to understand.
We highlight “ease of use” first because, without this, your patient monitoring program is a goner.
As for healthcare professionals, this factor relates more to how easy the setup and the actual act of monitoring is. There are some patients that your staff has to essentially sell on the whole concept. So, it's better for everyone if the devices are straightforward and cause no issues.
Bluetooth vs. Cellular
Another factor you need to watch out for when selecting remote patient monitoring devices is whether it has Bluetooth or cellular connectivity. Why does that matter?
Because that blood pressure reading your patient was excited about won’t matter when the Bluetooth won’t connect again.
You see, many monitoring devices do a great job when it comes to the ease of getting a reading, but they need to connect to wifi or a wifi-connected device to go any further. In contrast, cellular devices have to connect to nothing.
They simply transport the reading to that centralized interface we mentioned earlier.
Well, then, why is Bluetooth still used if it’s so inferior? Honest answer? It’s cheaper. When you question remote patient monitoring services on the actual devices your patients will have to use, be skeptical if you notice the word “Bluetooth technology” anywhere in their information.
Live Interaction
The next factor to consider is live interaction. This is the ability of providers to look at the incoming/existing health information at any time, anywhere, regardless of where the information is coming from. For example, they should be able to look at a reading that was taken at the patient's home. It’s called remote patient monitoring for a reason.
As much as we want all of your patient’s readings to be great and within safe boundaries, that will not always be the case. So, if a patient’s reading hits an unsafe point and needs addressing, you can communicate directly with that patient and advise on a course of action.
This point has more to do with the centralized interface side of things, but it’s still important to note. Imagine your patient’s heart rate is rising to dangerous levels. Do you really want them worrying about connecting to Wifi? Live interaction plays a part there.
Storage/Forwarding
Whenever we mention “centralized interface,” this is what we are talking about. The device should be able to instantly transfer the data and not be a barrier for the patient or the provider.
Remote Health Monitoring Devices Your Provider Should Offer
There are a lot of remote patient monitoring companies out there, which means they all offer unique experiences, devices, and services to your practice. In this section, we will walk you through the devices we offer.
Most practices, especially if they specialize, will just pick one device that collects to data most relevant to them.
While we offer only devices that are cellular, please be sure to actually look at the devices a remote patient monitoring company is providing. It’s not all that uncommon for providers to be given the run around when asking for actual visuals or examples, especially in relation to the monitoring interface.
Note: If you feel overwhelmed and have no idea where to start or what devices should be implemented in your patient monitoring program, don’t worry. You should go read this very in-depth guide on how you set up a Remote Patient Monitoring System.
.png?width=404&height=282&name=Blood%20Pressure%20Monitor%20(BP01).png)
Blood Pressure Monitor
When a patient is battling hypertension, it’s recommended that they take their blood pressure at the same time every day—sometimes even twice a day. Also, they have to be careful when they get a reading. There has to be some chunk of time between the reading and anything stimulating like drinking caffeine and exercising.
Our 4G Blood Pressure Monitor enables patients to take their blood pressure on their terms at whatever location works for them. Gone are the days when hypertensive patients have to come into the office to have their more official readings taken.
That never gave physicians an accurate picture of the patient’s situation, but this can. This monitor takes the reading and automatically transmits the data to the interface. It fills the gaps that were always a part of hypertensive care.
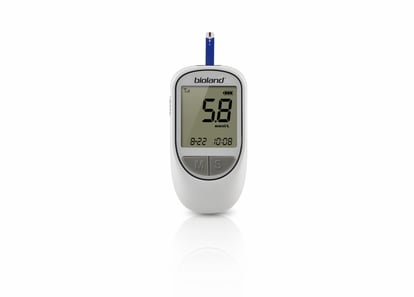
Glucose Meter
Diabetes is often called the “fickle disease.” It takes a lot of work and intervention to manage, and any diabetes patient will tell you they are always looking to make life easier without having to sacrifice the circumstances of their condition. It’s an extremely delicate line to balance.
Finger pricking is just one of the many inconveniences facing diabetic patients, so our Blood Glucose Meter is 4G enabled so that the patient can find out what their blood sugar is and move on. They don’t have to stop their lives (again) and worry about connecting to a wifi-enabled device to keep their blood glucose readings up to date.
It’s handled for them.
Thermometer & Pulse Oximeter
Yes, these are two separate devices, but they’re often part of a package deal. Before the pandemic, temperature and O2 readings were only done in a clinical setting, but that has drastically changed, like so many other things.
While a handful of chronic conditions require regular temperature and O2 readings to understand, these devices are rarely used alone.
Rather, they are used in tandem with other remote patient monitoring devices to fill the gaps in patient data. And with a condition like COVID-19, they are used to monitor risk.
And as we have mentioned with all of the other devices, these two are cellular-enabled as well—very helpful in the age of “quarantine” and “six feet apart.”
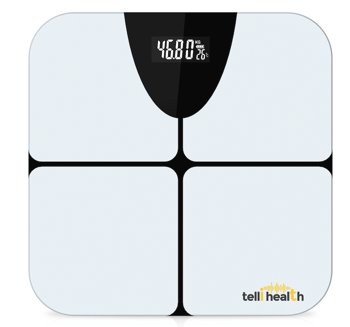
Weight Scale
While some remote patient monitoring devices are just your classic readers done better, the weight scale we are talking about is a little bit different. For example, most digital scales cap out at 300-400 lbs. So, if you are over that weight, you have to use an analog scale or find a “special” digital scale.
Thankfully, this is no longer the case. The weight scale we offer to everyone has a 600 lbs (272 kg) capacity. That way, none of your patients in higher-weight classes have to deal with yet another thing that alienates them or sets them aside.
Sleep and Resting Heart Rate Monitor
There are wearable devices that can track sleep, but they all tend to have different parameters when compared to others. If you don’t believe us, try wearing a Fitbit and an Apple watch when you sleep and see how different the data is.
The nonintrusive Sleep Monitor will automatically transmit patient data directly into the existing electronic health record, available to their provider immediately – a departure from traditionally cumbersome medical devices that require patients to manually track and record all readings.
All of that is to say; you might not be familiar with this remote patient monitoring device. It’s exactly what it sounds like. It’s the first cellular-enable sleep monitor mat of its kind that measures
- Sleep time
- Heart rate
- Sleep cycles (REM, deep, and light)
- Interruptions
- Sleep latency
- Waking
We all understand the importance of good sleep in relation to health and well-being, and it’s about time we were able to track it.
FDA Standards for Remote Patient Monitoring Devices
One of the most important prerequisites for devices used in healthcare is FDA compliance, and it makes sense, right? Patients must be protected from inconsistencies, manufacturing issues, etc. But this means there are a lot of rules to navigate, specifically when it comes to remote patient monitoring and the devices we use.
Here at Accuhealth, we know you have roughly 20,000 problems to solve every minute, so we work very hard not to let FDA compliance of your remote patient monitoring devices be #20,001.
You need to watch out for this when selecting devices because even though all remote patient monitoring devices need to comply with security and privacy regulations in HIPAA, technically, not all of them meet FDA standards.
A remote patient monitoring device is technically considered to be a wireless medical device, as per the FDA, and they have provided some helpful guidance on wireless medical devices as a whole and the FDA-recognized standards that are specifically related to wireless medical devices. You can find those standards by clicking here.
What Else Should Remote Patient Monitoring Companies Provide
At the end of the day, the remote patient monitoring company you work with needs to be doing everything they can to look out for you. Yes, that means FDA compliance, but that also includes consideration of things like physiological parameters, logistics, and reimbursement.
Note: In our guide on how to set up your remote patient monitoring program, we explain how you develop two different kinds of programs; full-service and self-managed. As we discuss measures that should be taken by your remote patient monitoring provider, we are specifically covering full-service programs.
Physiological Parameters
There are plenty of devices out there that will measure all sorts of physiological parameters, but it’s imperative that the device you offer accurately collects the measurements you require. There may be circumstances where an RPM device may be marketed to address a specific ailment or condition yet doesn’t capture specific data that you need to treat the condition.
You might think that’s common sense, but we have seen a lot of practices get a new gadget that does basically everything. The problem is that that does not mean it does any one thing well, especially not the one you need.
Logistics
If your patients encounter any sort of speed bump on their way to getting a reading, your program is going to have problems. So we recommend you support the tasks around patient measurement to make the experience completely seamless.
For instance, the best RPM devices offer shipping and tracking. They also offer easy returns and cleaning. While these sorts of tasks may seem minor in the grand scheme of things, they make the RPM experience that much easier for patients and healthcare providers.
Reimbursement
This is a big one. Without reimbursement, remote patient monitoring can quickly become unsustainable. In the proposed CMS changes for 2023, these got adjusted a bit, so be sure to read this to stay up to date on what is coming.
That being said, one key element for reimbursement is that the RPM device is considered to be a “medical device” per the FDA. We discussed FDA compliance before, but we bring it up again to highlight its importance.
While your remote patient monitoring devices don’t need to be FDA-approved, investing in an RPM device that is FDA-approved can give you more confidence that you will be reimbursed. By clicking here, you can find additional guidance on reimbursement, including the relevant CPT codes.
Finding Great RPM Devices
Remote patient monitoring’s backbone is the quality and dependability of its devices. As the technology stands now, if your devices stand up to the conditions listed above, you are in a place to deliver the best possible care.
Good devices play into the overall improvement of health outcomes. They also make life much easier for providers. Remote patient monitoring is supposed to be a solution, not a window to even more problems. The devices are the same.
Make sure that the patient monitoring devices your practice provides are ones you can stand behind, educate patients on, and use for the long haul. We heavily encourage you to keep these insights in mind when searching for your next RPM device.
Additional Resources
If reading this has just left you even more confused. We recommend taking a step back and starting from the beginning.
- How to Set Up Your Remote Patient Monitoring System
- The Complete Guide to Remote Patient Monitoring
If you are curious about CMS changes that may affect your practice, check this out.