Remote Patient Monitoring Certification and Training
For a limited time, sign up now and get exclusive access to our first online course: Introduction to Remote Patient Monitoring. Study the curriculum, learn the material and then take a short test to receive your Introduction to Remote Patient Monitoring Diploma to be officially certified by RPM U.
Remote Patient Monitoring University
in any Remote Patient Monitoring Program
Welcome to RPM U! Accuhealth's education center for healthcare providers who want a comprehensive understanding of RPM. Watch training videos; read RPM articles, real-world case studies and FAQs, listen to virtual care podcasts and much more.
Remote monitoring is officially the new staple medical service for delivering value-based healthcare. RPM is becoming a standard in both primary and specialty care.
Introduction to Remote Patient Monitoring Online Certification
in any Remote Patient Monitoring Program



Get your free education in Remote Patient Monitoring from the industry leader in RPM... you will receive a certificate upon completion of the course material.
Learning Objectives
in any Remote Patient Monitoring Program
The Introduction to Remote Patient Monitoring Course will teach you the following:
- Clearly understand what Remote Patient Monitoring (RPM) is
- Identify what to look out for when seeking RPM services
- Understand who pays for RPM devices and consumables
- Know the connectivity mechanism for RPM data transfer
- The various types of devices that are used in RPM
- Identify ways of tracking time spent by each patient in a month
- Understand what EHR integration is capable of doing
- Set out tips for achieving EHR integration
- Gain insight into the audits involved in delivering EHR services.
- Describe the compliance requirements for EHR systems
Choosing a Provider Is the First Step to Getting Started With Remote Patient Monitoring
in any Remote Patient Monitoring Program
Remote Patient Monitoring programs vary wildly between different providers. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet.
Choosing a Provider Is the First Step to Getting Started With Remote Patient Monitoring
in any Remote Patient Monitoring Program
Remote Patient Monitoring programs vary wildly between different providers. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet. Lorem ipsum dolor sit amet.
Remove WiFi and Bluetooth Dependence. They're Unreliable and Outdated.
The Telemonitoring devices used within any Remote Patient Monitoring program should be as simple as possible for patients to use. After all, patients will be using them on a daily basis.
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not require account management including logins and / or passwords
Plug-and-Play Devices are Required for Success in Any RPM Program
in any Remote Patient Monitoring Program
The Telemonitoring devices used within any Remote Patient Monitoring program should be as simple as possible for patients to use. After all, patients will be using them on a daily basis.
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not require account management including logins and / or passwords
Plug-and-Play Devices are Required for Success in Any RPM Program
in any Remote Patient Monitoring Program
The Telemonitoring devices used within any Remote Patient Monitoring program should be as simple as possible for patients to use. After all, patients will be using them on a daily basis.
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not require account management including logins and / or passwords
Plug-and-Play Devices are Required for Success in Any RPM Program
in any Remote Patient Monitoring Program
The Telemonitoring devices used within any Remote Patient Monitoring program should be as simple as possible for patients to use. After all, patients will be using them on a daily basis.
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not be dependent on Bluetooth or WiFi for connectivity
- Not require account management including logins and / or passwords
Course Modules

Understanding Remote Patient Monitoring

Understanding RPM Devices

How to Bill For RPM

EHR Integration

Audits & Compliance

Knowledge Test
3 Simple Steps to Get Certified

Step 1: Sign Up
Use the form above to sign up; we just need your name and email, and you will be automatically enrolled in the course! You can start right away.

Step 2: Complete the Course and Test
Completing the course will take you approximately 30 minutes, after which you will take a short knowledge test. You can stop and start at any time.

Step 3: Get Your Certificate
You will receive a certificate for the 'Introduction to Remote Patient Monitoring Course' after achieving 80% or greater on the knowledge test.
Enroll Now to Get Started
Registration for the course is quick, easy, and free for anyone to register. You will receive a certificate at the end of course.
RPM Guides & Whitepapers
Get valuable insight into how Accuhealth can increase patient engagement and health, resulting in measurable outcomes. From small family practices to Federally-Qualifed Health Centers (FQHC) we have solutions that can be tailored to every need.

White Paper
RPM Rescue
Get the FREE guide to reveal all of the essentials when selecting an RPM vendor, but also what to watch out for.

White Paper
The Practical Guide to Remote Patient Monitoring
Our practical guide was created to help healthcare providers setup a Remote Patient Monitoring program that will serve as a natural extension of your clinic's processes and procedures.

White Paper
Guide to RPM Success: Part 1 - Billing
Part 1: Billing - Everything You Need to Know To Increase Patient Engagement and Deliver Value-Based Care.
Case Studies
Remote Patient Monitoring has evolved over the years with the advent of new technologies and implementations of these technologies. At one time, RPM programs were seen as a novelty, but they are now considered the new staple medical service for providers looking to deliver value-based healthcare—particularly in primary and specialty care settings where providers interact closely with their patients.
RPM Rescue - How Remote Patient Monitoring is Saving Healthcare
Accuhealth + Athenahealth Marketplace Leadership

Tellihealth customizes RPM metrics to your goals, ensuring data drives decisions that matter—no one-size-fits-all approach.

While healthcare begins to rely more and more on tech, your organization’s wellbeing is truly dependent on the relationships existing within it.

Discover how personalized programs, patient-centered care, and flexible metrics create thriving RPM partnerships that transform healthcare delivery.

Learn how (CCM) drives success in value-based care contracts by improving patient outcomes, lowering costs, and strengthening care coordination.

Discover how nephrology practices can meet value-based care goals with tech-enabled solutions that simplify care delivery—without overloading providers.

Value-based care is a healthcare payment model that rewards providers for patient outcomes rather than volume of services.

Case Study
Levine Heart
Discover how Accuhealth's Remote Patient Monitoring enables Levine Heart & Wellness to provide proactive and attentive care.

Case Study
Telli Health
How Telli Health cellular-enabled devices improved accuracy and reliability for Accuhealth's rapidly growing remote patient monitoring program.

Case Study
Valley Medical Associates
The COVID-19 Pandemic created the opportunity to deploy high-touch care rapidly for the Valley Medical Team.

Case Study
Cribl LogStream
Accuhealth Leverages Cribl LogStream™, Brings Remote Patient Monitoring to Practices of All Sizes
Educational Content for Providers
Accuhealth attributes one of the driving forces of the success of our RPM program to be provider and patient education alike. To this end, we take great pride in providing detailed case studies, meticulously crafted training videos, webinars, and even a podcast for providers to learn more about the best way to implement an RPM program so that their clinic can see measurable outcomes. We've featured some of the most relevant highlights for providers below.
RPM Rescue - How Remote Patient Monitoring is Saving Healthcare
Remote Patient Monitoring Made Easy and Done Right®
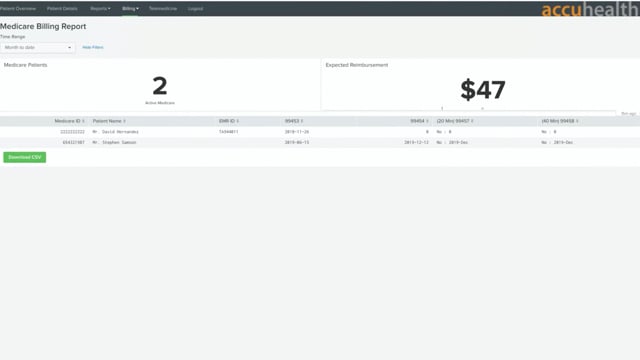
Accuhealth Medicare Billing Report Training Video
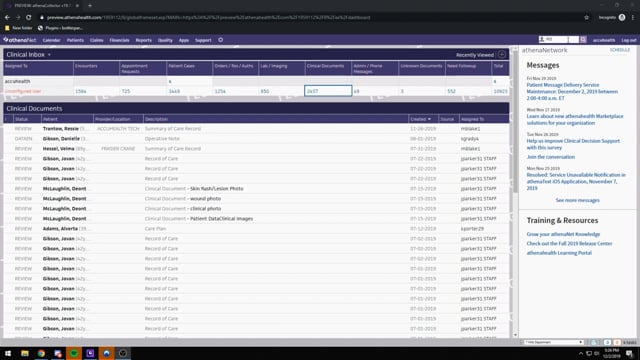
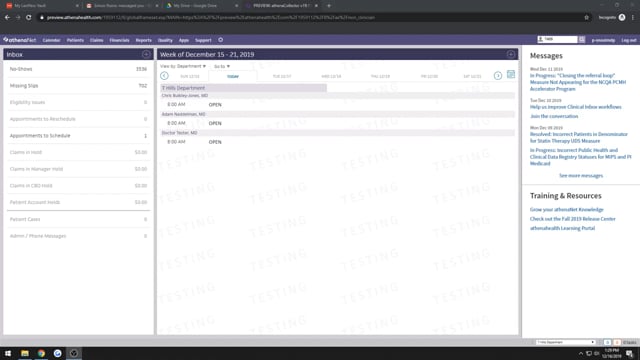
Where To Find Patient Vitals & Documents In Athena EMR
Accuhealth + Athenahealth Marketplace Leadership
.svg?noresize)
.svg?noresize)